Steven K. Wilson, MD, FACS, FRCS, presented “Changing Paradigms in Prosthetic Urology” during the 24th Annual Innovations in Urologic Practice on September 14, 2019 in Santa Fe, New Mexico.
How to cite: Wilson, Steven K. “Changing Paradigms in Prosthetic Urology” September 14, 2019. Accessed Jul 2025. https://grandroundsinurology.com/changing-paradigms-in-prosthetic-urology/
Changing Paradigms in Prosthetic Urology– Summary:
Steven K. Wilson, MD, FACS, FRCS, explores paradigm shifts in the materials and techniques used for inflatable penile prosthesis implants (IPP) and artificial urinary sphincters (AUS). He focuses on how urologists have improved standard of care through the use of new technology and a clearer understanding of the negative effects of these procedures.
Abstract:
The implantation of inflatable penile prostheses and urinary sphincters has been a part of the urologic armamentarium since Dr. F. Brantley Scott published the first clinical results of his devices in 1973. Scott’s work has proven unusually enduring, but changes have been made to his procedures over the past 46 years. Some were minor improvements, but others represent genuine paradigm shifts.
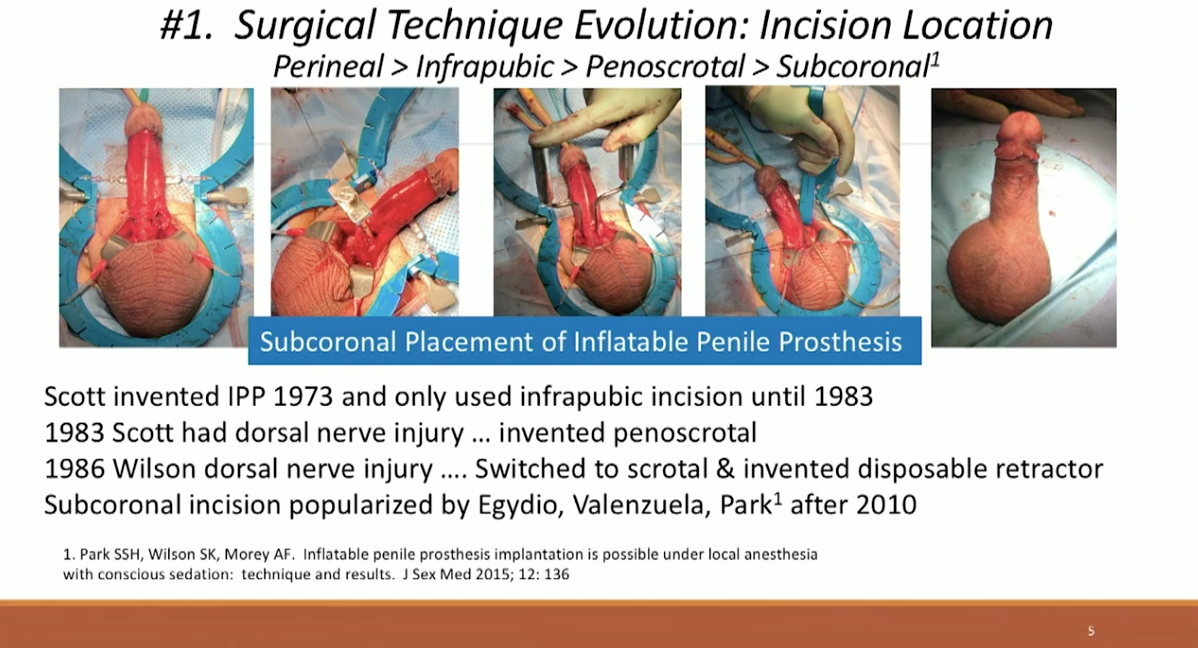
One major shift has been in surgical technique. In IPP implantation, the incision location has changed many times since 1973, from perineal to infrapubic to penoscrotal to subcoronal. The subcoronal incision, popularized in 2010 by Drs. Egydio, Valenzuela, and Park, has significant advantages, and is best for local anesthesia, Peyronie’s correction, lengthening and girth enhancement, and outpatient procedures.
The past decades have also seen a complete reversal from downsizing to upsizing of cylinders of IPP. While it was once traditional to undersize the cylinders, there is a documented trend in the US in favor of longer cylinders. Evidence suggests that deliberately oversized cylinders coincident with daily inflation results in larger penises.
Other paradigm shifts are in the area of AUS implantation. Many patients are rejecting traditional AUS, an implant which requires frequent revision, in favor of the “mini-jupette” graft for stress incontinence. It has proven to limit climacturia, as well as mild urinary leakage. AUS implantation itself is in the midst of a paradigm shift.
AUS patients are high-maintenance and experience recurrent incontinence. Urethral atrophy has long been viewed as the cause of this and efforts have been made to address this problem. However, current thinking holds that capsule formation and balloon fatigue are the true culprits. A pump that patients could deactivate at night could potentially radically lower the AUS revision rate. Ongoing work and research could continue to improve these old, but still fundamentally useful, procedures.
About the 24th Annual Innovations in Urologic Practice
Innovations in Urologic Practice (Innovations) is an annual, multi-day, CME-accredited conference devoted to innovative diagnostic and treatment strategies for and controversies related to some of the most common urologic problems in the current era. The topics covered include oncological management of the bladder, kidney, and prostate. The conference also emphasizes general urology topics in pelvic reconstruction and trauma, men’s health, and infections in the urology patient. Dr. Wilson presented this lecture during the 24th Innovations in 2019. Please visit this page in order to register for future Innovations meetings.
ABOUT THE AUTHOR
Steven K. Wilson, MD, FACS, FRCS, was formerly Professor of Urology at the University of Arkansas for Medical Sciences in Little Rock, Arkansas. The Steven K. Wilson Chair of Prosthetic Urology was endowed at this University in 2007. Through 46 years of practice and over 11,000 implants, he has performed urologic surgery in 53 countries and has been a visiting professor at several American training programs and numerous foreign centers.
He is the author or co-author of over 200 peer-reviewed publications, editorials, invited commentaries and abstracts, as well as 19 textbook chapters, countless surgical videos, and 5 prosthetic urology textbooks. He was the 2010 recipient of the St Paul’s Medal of the British Association of Urologic Surgeons, which is given yearly to a single urologist outside of the United Kingdom that has contributed significantly to world urology. In 2013, the F. Brantley Scott Award of Excellence was designated to Wilson. In 2017, he received the inaugural “Living Legend Award” of the Society of Urologic Prosthetic Surgeons. He has also been awarded lifetime achievement awards by the Alpha Omega Alpha Medical Honor Society, the AR Urologic Society, the Southeastern Section of the AUA, and the North Rhein-Westfalia Section of the German Urologic Society. He founded and remains Editor-in-Chief of the successful International Society of Sexual Medicine’s Video Journal of Prosthetic Urology.
Wilson is most recognized for his innovation of new surgical techniques, which have made the complex implantation of penile implants and sphincters minimally invasive. His notable literature contributions include strategies for infection and biofilm in penile prosthetics, the modeling procedure for Peyronie’s Disease, the single scrotal incision implantation of urinary sphincters, and the implantation of both IPP and AUS through a single scrotal incision and the ectopic placement of implant reservoirs. His current practice in La Quinta, California, is limited to prosthetic urology, and he continues to travel and teach others his techniques.