Seth R. Blacksburg, MD, MBA, presented “How Does Radiobiology Guide Treatment Options?” during the 23rd Annual Southwest Prostate Cancer Update on April 15, 2018 in Scottsdale, Arizona
How to cite: Blacksburg, Seth R. “How Does Radiobiology Guide Treatment Options?” April 15, 2018. Accessed [date today]. https://grandroundsinurology.com/how-does-radiobiology-guide-dose-fraction-and-source-selection/
How Does Radiobiology Guide Treatment Options? – Summary:
Seth Blacksburg, MD, MBA, argues that intensity-modulated radiation therapy (IMRT), brachytherapy, hypofractionation, and stereotactic body radiotherapy (SBRT) all have similar efficacy and safety for treating low and intermediate risk prostate cancer. However, patient and physician factors impact which modality will result in optimal outcomes in individual cases.
Macro Level Trends and Treatment Comparisons
The current NCCN guidelines on low and intermediate risk prostate cancer include many treatment options. While they are all beneficial options, certain modalities may be more appropriate depending on the physician and the treatment scenario.
Dr. Blacksburg illustrates the trends of radical prostatectomy (RP), radiotherapy, androgen deprivation therapy (ADT), and active surveillance utilization since 1990 through the CapSURE dataset. He compares survival and urinary and sexual function outcomes in RP versus observation through PIVOT data. Also, he reviews ten-year mortality and QOL outcomes following AS, RP, and radiotherapy through ProtecT data.
Treatment Options
Throughout this presentation, Dr. Blacksburg reviews the literature surrounding IMRT, brachytherapy, hypofractionation, and SBRT, their oncological benefits and toxicity risks, and factors, such as radiation dose and physician variability, that affect their curative and biochemical outcomes.
Notably, he discusses an article in the British Journal of Urology by Nelson N. Stone, MD and Richard G. Stock, MD, which proved that a higher biologically equivalent dose (BED) translated to improvement in biochemical outcomes. He reviews data from ASCENDE-RT, which was favorable toward brachytherapy, but remarks that because highly-experienced practitioners performed the treatments in this trial, it somewhat questions the legitimacy and durability of this particular modality.
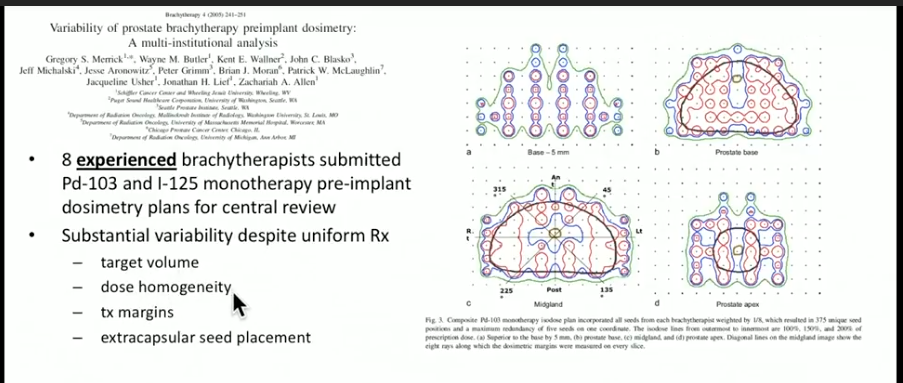
A multi-institutional analysis by Merrik et al. corroborated this idea. It followed eight experienced brachytherapists who submitted 32 preimplant dosimetry plans for central review. Despite the uniform prescription doses, the target volume, dose homogeneity, treatment margins, and the concept of using extracapsular seed placement greatly varied between experts.
While brachytherapy, IMRT, and hypofractionation are established treatments, SBRT is relatively new. Clinicians need more mature, quality data to properly assess SBRT against these other modalities. Additionally, results published in high impact factor publications often guide patients’ treatment decisions. Therefore, Dr. Blacksburg suggests that new SBRT data needs to appear in higher-impact factor publications. Currently, the highest-impact publication on SBRT, in the Journal of Clinical Oncology, was a negative toward the modality.
Analysis of Treatment Options
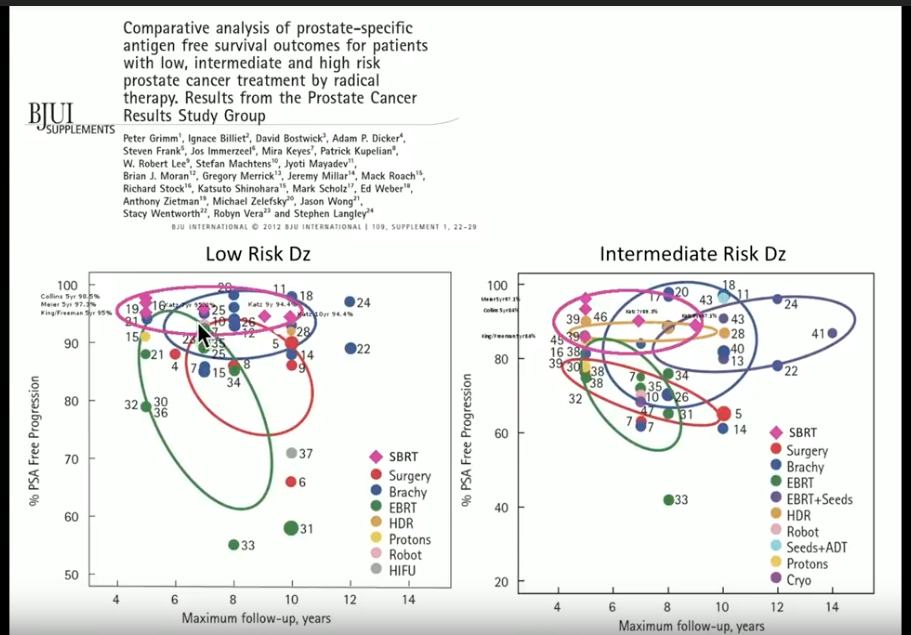
A comparative analysis study by Grimm et al. assessed patient outcomes according to PSA free survival and compared between treatment with surgery, brachytherapy, EBRT, EBRT plus seeds, HDR brachytherapy, robotic prostatectomy, seeds plus androgen deprivation therapy (ADT), high-intensity focused ultrasound (HIFU), cryotherapy, as well as others based on risk level. Dr. Blacksburg added the pink value to represent SBRT in this figure (left) to argue that they are all good treatment options.
Physician and Patient Selection
Although physicians tend to focus on curing the patient’s disease, patients often have QOL priorities, such as cure, salvage options, incontinence, burns, bowel problems, and length of treatment, when making treatment decisions. When choosing a modality, physicians must always consider the trade-off of convenience, invasiveness, toxicity, and efficacy.
Paradigm Change in Prostate Cancer Treatment
Although urologists as a whole used to treat prostate cancer patients with the sole intent to cure, they now do not trivialize the importance of patient QOL. The search for and application of more accurate biopsy and imaging techniques, as well as better post-RT salvage techniques, reflects this paradigm shift.