How to cite: Flavell, Robert “Incorporating New PET Imaging and Theranostic Approaches into Prostate Cancer Practice | Interesting Cases ” June 1, 2018. Accessed [date today]. https://grandroundsinurology.com/incorporating-new-pet-imaging-and-theranostic-approaches-into-prostate-cancer-practice-interesting-cases/
Incorporating New PET Imaging and Theranostic Approaches into Prostate Cancer Practice | Interesting Cases – Summary:
In part two of this two-part series, an oncologist, urologist, and nuclear medicine physician review four distinct prostate cancer cases, sharing their thoughts and recommendations with regard to the use of recently developed imaging agents and therapies, including PSMA-based agents, fluciclovine, and 223Ra. Cases include patients at several stages, such as initial diagnosis, biochemical recurrence, and castrate-resistant prostate cancer.
Robert R. Flavell, MD, offers an introductory overview of theranostics and advances in nuclear imaging and therapies, especially prostate-specific membrane antigen (PSMA) agents. Subsequently, he leads a panel with Susan F. Slovin, MD, PhD, E. David Crawford, MD, and Phillip J. Koo, MD in reviewing four distinct prostate cancer cases, sharing their thoughts and recommendations with regard to use of recently developed imaging agents and therapies.
This panel discussion is part two of a two-part series. Part one is: “Incorporating New PET Imaging and Theranostic Approaches into Prostate Cancer Practice.”
View Part I
The Role of Imaging During the Course of Prostate Cancer Progression
At this time, rapidly advancing positron-emission tomography (PET) imaging and theranostic approaches are changing the way physicians treat patients.
As an illustration of the role imaging plays in managing prostate cancer, Dr. Flavell presents a simplified timeline of the typical interventions physicians perform during the course of disease, describing imaging performed at the time of initial diagnosis, biochemical recurrence, and progression to castration-resistant prostate cancer (CRPC).
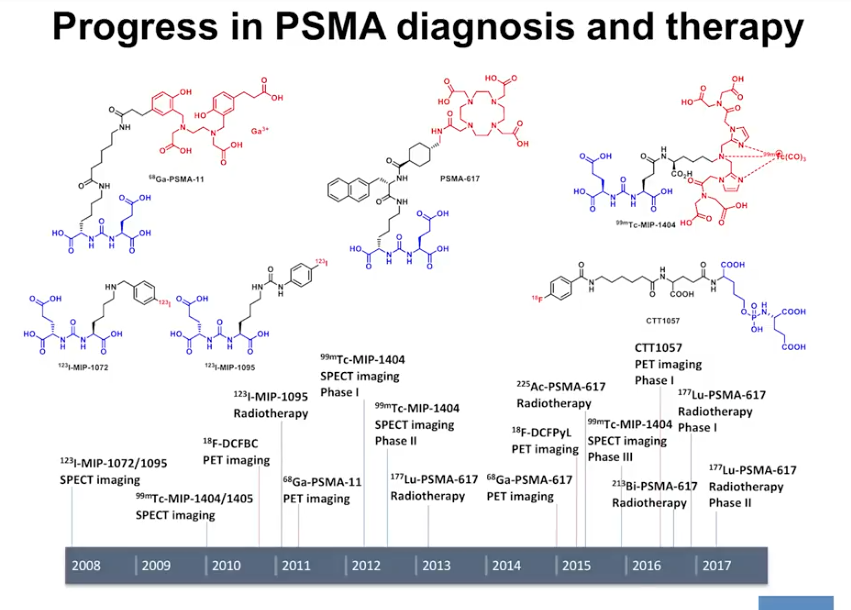
Next Generation Nuclear Imaging and Therapy Approaches
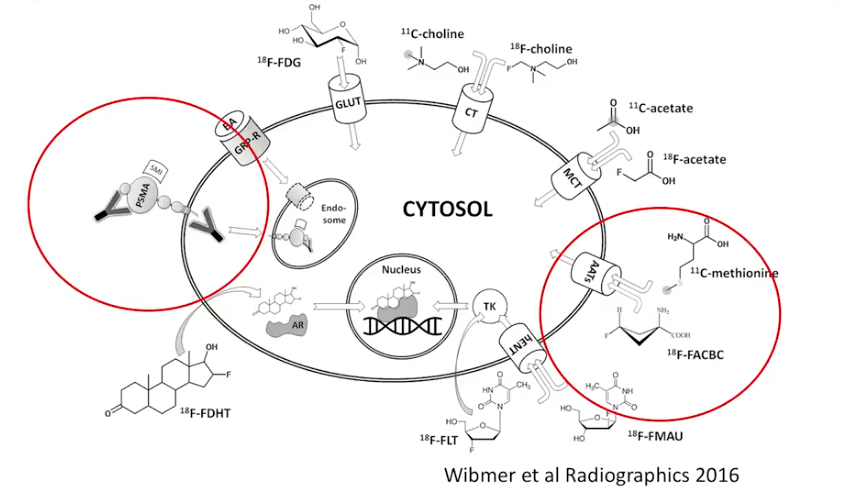
While a multitude of new nuclear medicine and positron-emission tomography (PET) imaging agents have emerged in recent years, Dr. Flavell focuses this discussion on PSMA agents and fluciclovine.
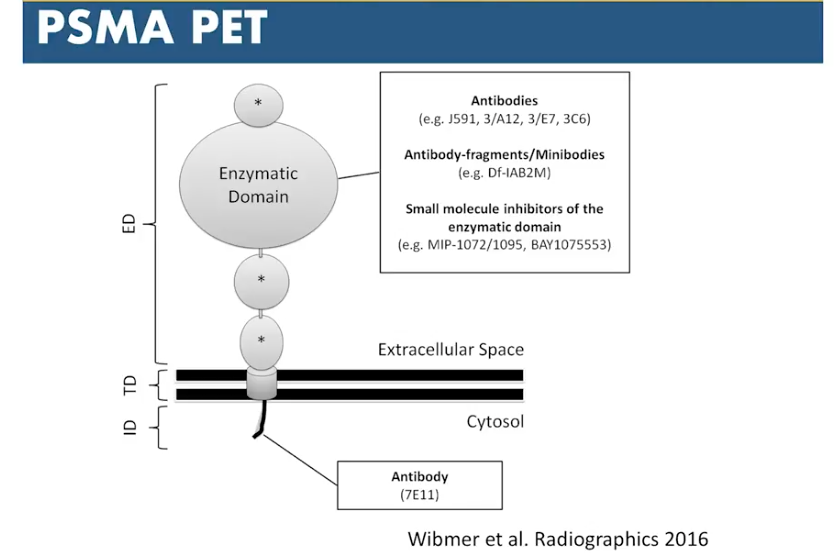
PSMA
Currently, there are many diagnostic PSMA agents, notably gallium-68 and 18F-PSMA-1007. However, all PSMA agents are still investigational. PSMA often expresses in areas that are not prostate cancer, such as neovasculature in benign and malignant tumor subtypes. Also, PSMA sometimes expresses in normal variants, like cervical and stellate ganglion. Therefore, if physicians see PSMA uptake in solitary bone lesions or unexpected locations, they should beware of false positives or consider other tumors.
Although PSMA is arguably the most sensitive imaging option available for detecting metastatic disease in newly-diagnosed intermediate to high-risk prostate cancer, it still misses a significant portion of micrometastatic disease. It is unclear what role PSMA has in changing management, but it looks promising for guiding radiation planning and identifying distant metastatic disease.
Fluciclovine
Fluciclovine is a non-naturally occurring amino acid PET radiotracer, recently FDA-approved for detection of suspected recurrent prostate cancer. It is also highly sensitive for prostate cancer recurrence. Unlike many other radiopharmaceuticals, this agent is rapidly exported from cells, so imaging must occur very shortly after injection.
Panel Discussion
During the second half of this presentation, Dr. Flavell leads Dr. Slovin, a medical oncologist, Dr. Crawford, a urologist, and Dr. Koo, a nuclear medicine physician, in examining the efficacy of new PET imaging approaches through a case-based format. With this intention, the panelists review four cases, including a patient initially diagnosed with high-risk prostate cancer, two patients with biochemical recurrence post-radical prostatectomy and salvage radiotherapy, and a patient with CRPC.
Conclusion
Following the panel discussion, Dr. Flavell provides a brief overview of radium-223 and the ALSYMPCA trial, the concept of theranostics and lutetium-177, and alpha emitters.
ABOUT THE AUTHOR
Dr. Flavell is the Chief of Molecular Imaging and Therapeutics Clinical Section in the Department of Radiology and Biomedical Imaging at the University of California, San Francisco (UCSF). He is also an Assistant Professor of Radiology at UCSF. Dr. Flavell received his medical degree from Weill Cornell Medical College, and his PhD from Rockefeller University as part of the Tri-Institutional MD-PhD program. He completed his one-year internship at Memorial Sloan Kettering Cancer Center in New York. Dr. Flavell then went on to complete a four-year Diagnostic Radiology Residency at UCSF, where he also finished a Nuclear Medicine Fellowship.
Dr. Flavell is an expert in nuclear medicine, molecular imaging, and therapeutics. His laboratory, the Molecular Imaging Lab, focuses on the development of new molecular imaging tools for better understanding of disease progression in patients with prostate and other cancers. Dr. Flavell is an author on over 50 peer-reviewed publications and has been widely recognized for his research.